FET Protocol (Frozen Embryo Transfer) – Advantages, Methods, and Effectiveness
FET protocol (aka Cryoprotocol) is the transfer of embryos that were frozen in the previous cycle to the uterus.
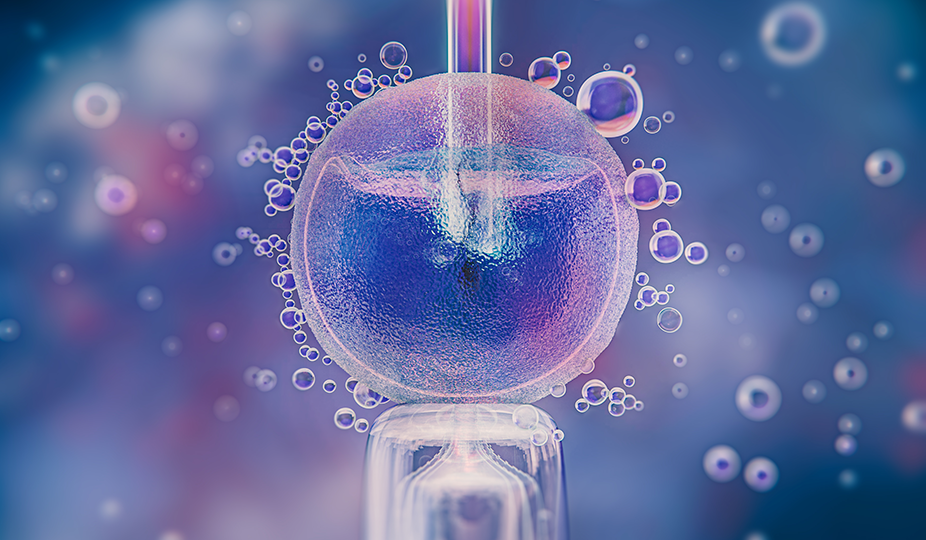
FET protocol, or IVF cryopreservation, is a vital procedure in assisted reproductive technology that involves freezing embryos from a previous cycle for future use. It can be performed in natural and hormone-prepared cycles, depending on the patient’s specific circumstances.
Sunshine fertility experts have consulted reproductive specialists to tell you more about how the FET protocol works, how to prepare for FET, how frozen embryo transfer differs from the same procedure with fresh embryos, and what the success rates are.
Applications of Cryopreservation in IVF
Reproductologists suggest you use the FET protocol in one of the three major cases: as a backup, for the future, or in case of delays.
- Ensuring a backup of embryos in case of an unsuccessful attempt: If the initial cycle fails, frozen embryos can be thawed and utilized in a shortened cycle to continue the program.
- Future family planning: Cryopreservation allows couples and individuals to preserve embryos for future attempts to have more children.
- Delayed transfer due to specific conditions: Cryopreservation is useful when the woman’s endometrium or hormonal background is not suitable for immediate embryo transfer after fertilization, requiring a waiting period of one or more cycles.
Success Rates of Cryopreservation FET Protocols
The probability of achieving pregnancy using cryopreservation protocols is higher compared to using “fresh” embryos. With Sunshine programs, pregnancy on average occurs in 70% of cases involving cryopreserved embryos. This increased success rate is attributed to the selective transfer of the best embryos developed up to 4-5 days during cryopreservation.
Additionally, synchronization of endometrium and embryo development stages is achieved without stimulation using gonadotropins, enhancing the implantation frequency. Cryopreservation FET protocols are particularly effective for women under 35 with tubal infertility.
It is important to mention, that all our FET programs obligatory imply hormone tests, ovulation presence, or hCG levels before implementing the cryopreservation protocol. The timing and stage of embryo development during cryopreservation are carefully evaluated to prepare the endometrium for the subsequent embryo transfer.
Different Cryopreservation Methods – Slow vs Rapid Freezing
Cryopreservation protocols involve specific hormone administration schemes to prepare the endometrium before frozen embryo transfer. Two commonly used freezing methods are slow freezing (software) and ultra-rapid (vitrification).
| Slow computer-controlled freezing | Vitrification | |
|---|---|---|
| Time | More than 3 hours | Less than 10 minutes |
| Ice crystal formation risk | High | Low |
| Mechanical damage | More | Less |
| Chemical damage | Less | More |
| Cost | More expensive | Less expensive |
| Speed of freezing | -0.3 degrees C/minute | -23 degrees C/minute |
| Sample volumes | 100-250 ml | 1-2 ml |
Slow computer-controlled freezing is still widely used all around the world. It implies step-by-step temperature lowering up to -196 degrees to prevent ice crystal formation. At our affiliated clinics, we also utilize the modern vitrification method, which ensures optimal cell quality preservation. Vitrification (rapid freezing) allows the freezing of embryos at any stage of development with minimal damage. Embryos are stored in labeled plastic straws submerged in liquid nitrogen, enabling long-term storage of over 10 years.
Indications for Embryo Cryopreservation
- Preservation of high-quality embryos remaining after the initial transfer for future use.
- Inability to transfer embryos in the current cycle due to the patient’s clinical condition.
Advantages of Cryopreservation Protocols
- Reduced medication load on the woman’s body.
- No need for follicle puncture.
- Lower cost compared to standard IVF programs.
Types of Cryopreservation Protocols
Cryopreservation in the Natural Cycle (EC)
This protocol involves utilizing frozen embryos for fertilization without hormone use, mimicking a natural cycle. Hormonal medications are prescribed only a few days before and after embryo transfer to support the luteal phase. It is suitable for patients who ovulate regularly, have regular menstrual cycles, or are young. The growth of the dominant follicle and endometrium is monitored through ultrasound, and hormone analysis may be conducted if necessary. Once ovulation is confirmed, thawed embryos are transferred to the uterus. Sunshine Agency has extensive experience in conducting cryopreservation protocols in the natural cycle.
Cryopreservation on Hormone Replacement Therapy (HRT)
This protocol creates an artificial menstrual cycle supplemented with hormonal agents to control reproductive processes. It is beneficial for patients with irregular menstrual cycles, anovulation, decreased ovarian reserve, no ovaries, women over 35, women with insufficient endometrial thickness in the natural cycle, and those with decreased or depleted ovarian function. The scheme for the cryopreservation protocol on HRT involves taking estrogen from the first days of the menstrual cycle, monitoring endometrial growth through ultrasound, administering progesterone when the endometrium reaches the optimal thickness and structure, embryo transfer based on the stage of frozen embryos, and hormone support after the transfer (duration determined by the doctor).
Cryopreservation in a Stimulated Cycle
This program is designed for patients who require small doses of gonadotropins to stimulate ovulation due to insufficient endometrial growth in a natural cycle or HRT. Once the follicle reaches the desired size (18-20 mm) and the endometrium has the ideal thickness, hCG is administered, followed by the transfer of thawed embryos 4-5 days later.
Before the FET Cycle: Preparing the Canvas
Imagine that you are standing on the threshold of your FET journey. Let’s begin with meticulous preparation to ensure the optimal conditions for embryo implantation. Here’s what you can expect.
1. Ovarian Activity Suppression
For starters, doctors will prescribe you medications to reduce ovarian activity. This typically involves either taking birth control pills or receiving an injection of a hormone called leuprolide, commonly known as Lupron. This initial phase aims to create a controlled environment in your reproductive system.
2. Estradiol Introduction
After approximately ten days of ovarian activity suppression, you will have to take the hormone estradiol. It can be in the form of a pill, injection, or patch. Estradiol plays a crucial role in preparing the endometrium (the lining of the uterus) to be receptive to the embryo.
3. Monitoring
Throughout this process, doctors will take regular blood tests to measure your estradiol levels. Around two weeks after starting estradiol, they will do a vaginal ultrasound. This ultrasound helps determine whether your endometrial lining has reached an appropriate thickness for embryo transfer.
4. Progesterone Usage
When your endometrium is deemed ready and your estradiol levels are optimal, your doctor will instruct you to begin using progesterone. Progesterone can be taken as an intramuscular injection, vaginal gel, or pill, and the method chosen will depend on your specific circumstances. The timing of progesterone administration is meticulously planned to align with the thawing and transfer of your frozen embryos.
5. Medrol
Additionally, you will be prescribed Medrol, a steroid medication that can aid in embryo implantation. Medrol is typically taken over a five-day period.
6. Continued Medication
It’s essential to continue taking estradiol and progesterone until your doctor instructs you to stop. If you become pregnant, you may be advised to continue these medications until you are at least ten weeks along.
Embryo Handling and Selection
During the FET process, your frozen embryos play a crucial role. Here’s a brief overview of what happens with your embryos.
- Embryos are frozen at different developmental stages, such as day 1, day 3 (cleavage stage), or day 5 (blastocyst stage), depending on your specific situation. These embryos are stored individually or in groups within small vials or straws. The number of vials or straws thawed for your FET is determined by factors like your age, embryo quality, the number of embryos per vial/straw, and other considerations that were relevant at the time of freezing.
- It’s important to note that some embryos may not survive the thawing process. Your embryologist will assess your unique circumstances and recommend the number of embryos to thaw and transfer.
- In some cases, additional laboratory steps may be required for your embryos to grow and develop after thawing before they can be placed in your uterus. These additional steps, if necessary, can impact the cost and timeline of your FET cycle.
As you see, the FET cycle involves meticulous planning, medication management, and precise handling of frozen embryos. Sunshine’s healthcare team will guide you through each step, ensuring that you have the best chance of achieving a successful pregnancy while prioritizing your health and well-being. If you have any questions or concerns about your FET cycle, don’t hesitate to discuss them with your healthcare provider.
Risks and Possible Complications During FET
Even though both methods of embryo freezing are mastered by modern reproduction clinics, there are risks.
Physical Discomfort
The FET procedure is invasive and can lead to unpleasant side effects like cramping, bloating, and bleeding.
Embryo Survival
There is a chance that some of your frozen embryos won’t make it through the thawing process. If you have a few embryos and none of them survive the procedure, you won’t have the material for the IVF.
Multiples
You can transfer multiple embryos to increase the IVF success rate. However, it means that you can get pregnant with multiple babies at the same time, which puts an additional load on your uterus and body as a whole. Multiple pregnancies have a higher risk of premature newborns due to preterm labor, they also often require C-section.
FET Protocol Success Rate Is Never 100%
Unfortunately, doctors and fertility experts cannot guarantee that the procedure will succeed and result in pregnancy even if all conditions have been met and all stages of the protocol have been completed.
FET Protocol FAQ:
Cryopreservation protocols offer benefits such as reduced medication load, no follicle puncture, and lower costs compared to standard IVF programs.
The main types of cryopreservation protocols are cryopreservation in the natural cycle (EC), cryopreservation on hormone replacement therapy (HRT), and cryopreservation in a stimulated cycle.
Cryopreservation in the natural cycle is suitable for patients who ovulate regularly, have regular menstrual cycles, or are young.
Cryopreservation on hormone replacement therapy is beneficial for patients with irregular menstrual cycles, anovulation, decreased ovarian reserve, no ovaries, women over 35, women with insufficient endometrial thickness in the natural cycle, and those with decreased or depleted ovarian function.
Cryopreservation in a stimulated cycle involves administering small doses of gonadotropins to stimulate ovulation when the endometrial growth is insufficient. Once the desired follicle size and endometrial thickness are achieved, the embryos are thawed and transferred.